Sciatica
Definiton of Sciatica
The term sciatica describes a symptom rather than a specific disease. Some use it to mean any pain starting in the lower back and going down the leg. Others use the term more specifically to mean a nerve dysfunction caused by compression of one or more lumbar or sacral nerve roots from a spinal disc herniation. Pain typically occurs in the distribution of a dermatome and goes below the knee to the foot. It may be associated with neurological dysfunction, such as weakness. The pain is characteristically of shooting type, quickly traveling along the course of the nerve.
Causes of Sciatica
Spinal disc herniation
Spinal disc herniation pressing on one of the lumbar or sacral nerve roots is the primary cause of sciatica, being present in about 90% of cases.
Sciatica caused by pressure from a disc herniation and swelling of surrounding tissue can spontaneously subside if the tear in the disc heals and the pulposus extrusion and inflammation cease.
Spinal stenosis
Other compressive spinal causes include lumbar spinal stenosis, a condition in which the spinal canal (the spaces the spinal cord runs through) narrows and compresses the spinal cord, cauda equina, or sciatic nerve roots. This narrowing can be caused by bone spurs, spondylolisthesis, inflammation, or herniated disc, which decreases available space for the spinal cord, thus pinching and irritating nerves from the spinal cord that travel to the sciatic nerves.
Piriformis syndrome
Piriformis syndrome is a controversial condition that, depending on the analysis, varies from a “very rare” cause to contributing to up to 8% of low back or buttock pain. In 15% of the population, the sciatic nerve runs through, or under the piriformis muscle rather than beneath it. When the muscle shortens or spasms due to trauma or overuse, it’s posited that this causes compression of the sciatic nerve. It has colloquially been referred to as “wallet sciatica” since a wallet carried in a rear hip pocket compresses the buttock muscles and sciatic nerve when the bearer sits down. Piriformis syndrome cause sciatica when the nerve root is normal.
Pregnancy
Sciatica may also occur during pregnancy as a result of the weight of the fetus pressing on the sciatic nerve during sitting or during leg spasms. While most cases do not directly harm the fetus or the mother, indirect harm may come from the numbing effect on the legs, which can cause loss of balance and falling. There is no standard treatment for pregnancy induced sciatica.
Other
Sciatica can also be caused by tumours impinging on the spinal cord or the nerve roots. Severe back pain extending to the hips and feet, loss of bladder or bowel control, or muscle weakness may result from spinal tumours or cauda equina syndrome. Trauma to the spine, such as from a car accident, may also lead to sciatica.
Signs and Symptoms of Sciatica
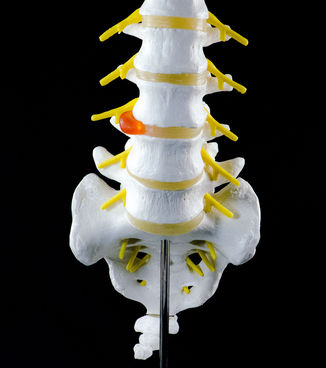 Sciatica is a set of symptoms including pain caused by general compression or irritation of one of five spinal nerve roots of each sciatic nerve—or by compression or irritation of the left or right or both sciatic nerves. Symptoms include lower back pain, buttock pain, and pain, numbness or weakness in various parts of the leg and foot. Other symptoms include a “pins and needles” sensation, or tingling and difficulty moving or controlling the leg. Typically, symptoms only manifest on one side of the body. The pain may radiate below the knee, but does not always.
Sciatica is a set of symptoms including pain caused by general compression or irritation of one of five spinal nerve roots of each sciatic nerve—or by compression or irritation of the left or right or both sciatic nerves. Symptoms include lower back pain, buttock pain, and pain, numbness or weakness in various parts of the leg and foot. Other symptoms include a “pins and needles” sensation, or tingling and difficulty moving or controlling the leg. Typically, symptoms only manifest on one side of the body. The pain may radiate below the knee, but does not always.
Risk Factors for Sciatica
- Age: The spine and the body in general begins to experience degeneration as people are getting older.
- Obesity: Obesity causes to increase the strees on your spine which triggers sciatica.
- Occupation and sports: The repeated contraction of a muscle in the hip called the piriformis muscle used in walking and running can causes irritation to the sciatic nerve. Also, a job that requires you to twist your back, carry heavy loads may be one of the risk factors.
- Sitting for long periods of time: Who sit at a computer all day or drive a vehicle for a long time may have sciatica because sitting for a long time increase the pressure on the sciatic nerve.
- Diabetes: Diabetes increases the risk of nerve damage by affecting the way the body uses blood sugar.
- Pregnancy: Hormonal changes and the position of the baby may increaase the risk of sciatica.
Diagnosis of Sciatica
Sciatica is typically diagnosed by physical examination, and the history of the symptoms. Generally if a person reports the typical radiating pain in one leg as well as one or more neurological indications of nerve root tension or neurological deficit, sciatica can be diagnosed.
The most applied diagnostic test is the straight leg raise to produce Lasègue’s sign, which is considered positive if pain in the distribution of the sciatic nerve is reproduced with between 30 and 70 degrees passive flexion of the straight leg. While this test is positive in about 90% of people with sciatica, approximately 75% of people with a positive test do not have sciatica.
Imaging tests such as computerised tomography or magnetic resonance imaging can help with the diagnosis of lumbar disc herniation. The utility of MR neurography in the diagnoses of piriformis syndrome is controversial.
Prevention from Sciatica
- Be careful when lifting heavy objects. Get close to object. Keep a long spine and keep your arms close in to your body when lifting. Avoid lifting and twisting simultaneously.
- Exercise regularly but avoid the activities which causes irritation of your nerves and increases pressure on your muscles.
- Avoid sitting for a long time and choose a seat with good lower back support and arm rests.
Treatment of Sciatica
When the cause of sciatica is lumbar disc herniation, most cases resolve spontaneously over weeks to months. Initially treatment in the first 6–8 weeks should be conservative. There does not appear to be a significant difference in outcomes between advice to stay active and recommendations of bed rest. Similarly, physical therapy (exercises) has not been found better than bed rest.
Medication
Although medicines are commonly prescribed for the treatment of sciatica, evidence for analgesics is poor. Specifically, NSAIDs do not appear to improve immediate pain and all NSAIDs appear about equivalent. Evidence is also lacking in use of opioids and muscle relaxants. In those with sciatica due to piriformis syndrome, botulism toxin injections may improve pain and or function.
Surgery
Surgery for unilateral sciatica involves the removal of part of the disc, known as a discectomy. While it results in short term benefits, long term benefits appear equivalent to conservative care. Treatment of the underlying cause of the compression is needed in cases of epidural abscess, epidural tumors, and cauda equina syndrome.
Epidurals
Good quality of evidence to suggest short-term pain reduction with epidural steroid injections, long-term benefit is controversial. Other agents, ex: TNF inhibitors, have not shown efficacy in most randomized controlled trials.
Alternative medicine
Moderate quality evidence suggests that spinal manipulation is an effective treatment for acute sciatica. For chronic sciatica the evidence is poor. Spinal manipulation has been found generally safe for the treatment of disc-related pain; however, case reports have found an association with cauda equina syndrome and it is contraindicated when there are progressive neurological deficits.
